City of Houston offers you three (3) unique medical plans. All plans include preventive care services and a four-tier prescription drug plan. Full-time and part-time employees who consistently worked 30 or more hours per week over the past 12 months are eligible for benefits. The three (3) plans offered are the Cigna Open Access, the Cigna Limited Network, and the Consumer-Driven Health Plan (CDHP).
Medical Plan Options


Medical Plan Information
-
Important: Duplication of coverage is not allowed
If both you and your spouse work for the city, you may be covered as an employee or a retiree, or as a dependent — but not both. Dependents may be enrolled under only one parent or guardian.
Transparency in Coverage Rule
This link leads to the machine-readable files that are made available in response to the federal Transparency in Coverage Rule and include negotiated service rates and out-of-network allowed amounts between health plans and health care providers.
The machine-readable files are formatted to allow researchers, regulators and application developers to more easily access and analyze data.
Cigna Machine Readable Files
Cigna Open Access
What you want to know:
- Access to over 572,000 providers all over the United States, without having to list a primary care physician or request referrals to specialists
- Copays for doctor visits
- - $40 copay for primary care visit
- - $65 for a Tier 1 specialist/$80 for a non-tier specialist
- Deductible
- - $850 (individual) / $1,700 (family)
- Out-of-pocket maximum
- - $8,700 (individual) / $17,400 (family)
Need more information?
OAP Full Plan Documents
OAP Pharmacy Full Plan Documents
Limited Network Plan
What you want to know:
- Provider groups:
- - Kelsey-Seybold
- - Village Medical
- - Renaissance
- Copays for doctor visits
- - $35 copay for primary care visit
- - $65 copay for specialist visit
- Deductibles
- - For medical services: $200 (individual) / $600 (family)
- - For prescriptions: $150 (individual) / $450 (family)
- Out of pocket maximums
- - $8,700 (individual) / $17,400 (family)
Need more information?
Limited Network Plan Open Enrollment 2023 – What You Need to Know
Summary of Benefits (Limited Network)
Limited Network Full Plan Documents
Limited Network Pharmacy Full Plan Documents
Limited Physicians Directory
Renaissance Physicians Pamphlet
Village Medical Landing Page
Village MD Directory
Village MD Locations
Kelsey-Care
Consumer-Driven Health Plan
What you want to know:
- Includes a Health Reimbursement Account (HRA)
- - City of Houston pays the first $500 to $1,000 (for family) depending on coverage tier
- - Unused amounts rollover from previous plan year
- No copays = more out-of-pocket costs at the time of service
- - 20% coinsurance (in network) / 40% coinsurance (out of network)
- Deductibles
- - In network: $1,750 (individual) / $3,500 (family)
- - Out of network: $3,500 (individual) / $7,000 (family)
- Out-of-pocket maximums
- - In network: $8,700 (individual) / $17,400 (family)
- - Out of network: $17,400 (individual) / $34,800 (family)
Need more information?
Summary of Benefits (CDHP)
CDHP Full Plan Documents
CDHP Pharmacy Full Plan
Cigna Choice Fund HRA Information Flyer
Find a Doctor, Dentist or Facility
Download the myCigna app, or log into your myCigna.com portal for quick and easy access to providers in your area.
You may also call one of the on-site Cigna representatives. Please refer to the provider contact list for details.
Urgent Care Facilities
If you need medical attention, your first thought may be to go to the emergency room. But if your condition isn’t serious or life threatening, you have a less expensive option.
An urgent care center provides quality care like an emergency room, but can save you time and money. Visit an urgent care for things like minor cuts, burns and sprains, fever and flu symptoms, joint or lower back pain, and urinary tract infections.
Urgent care facilities accepted by all medical plans.
Convenience care facilities are for employees enrolled in the CDHP (HRA) & (OAP Full) plans only).
Pharmacy Plan
When it comes to filling your prescriptions, choice, convenience and cost are important to you. There are over 4,000 retail pharmacies in your network for 30-day prescriptions and 31,000 retail pharmacies for 90-Day prescriptions.
Free Medications
Preventive Generic Medications: Preventive medications are used to prevent conditions like high blood pressure, high cholesterol, heart attack, stroke, diabetes, asthma, prenatal nutrient deficiency, etc. The City’s prescription drug plan covers most of these medications at no cost to you. Go to myCigna.com website, app or call Cigna Express Scripts at 800-835-3784 to learn which medications are free. You can also use the Drug Cost tool to estimate costs of any medications that are not on the no cost list.
No Cost Smoking Cessation and Contraceptive Medications: The City’s pharmacy plan covers prescription and over-the-counter smoking cessation and contraceptive products with no copay, coinsurance or deductible.
Patient Assurance Program: Certain preferred brand insulin drugs are eligible for a maximum copayment of $25 for a 30-day supply and $75 for a 90-day supply at participating in-network pharmacies.
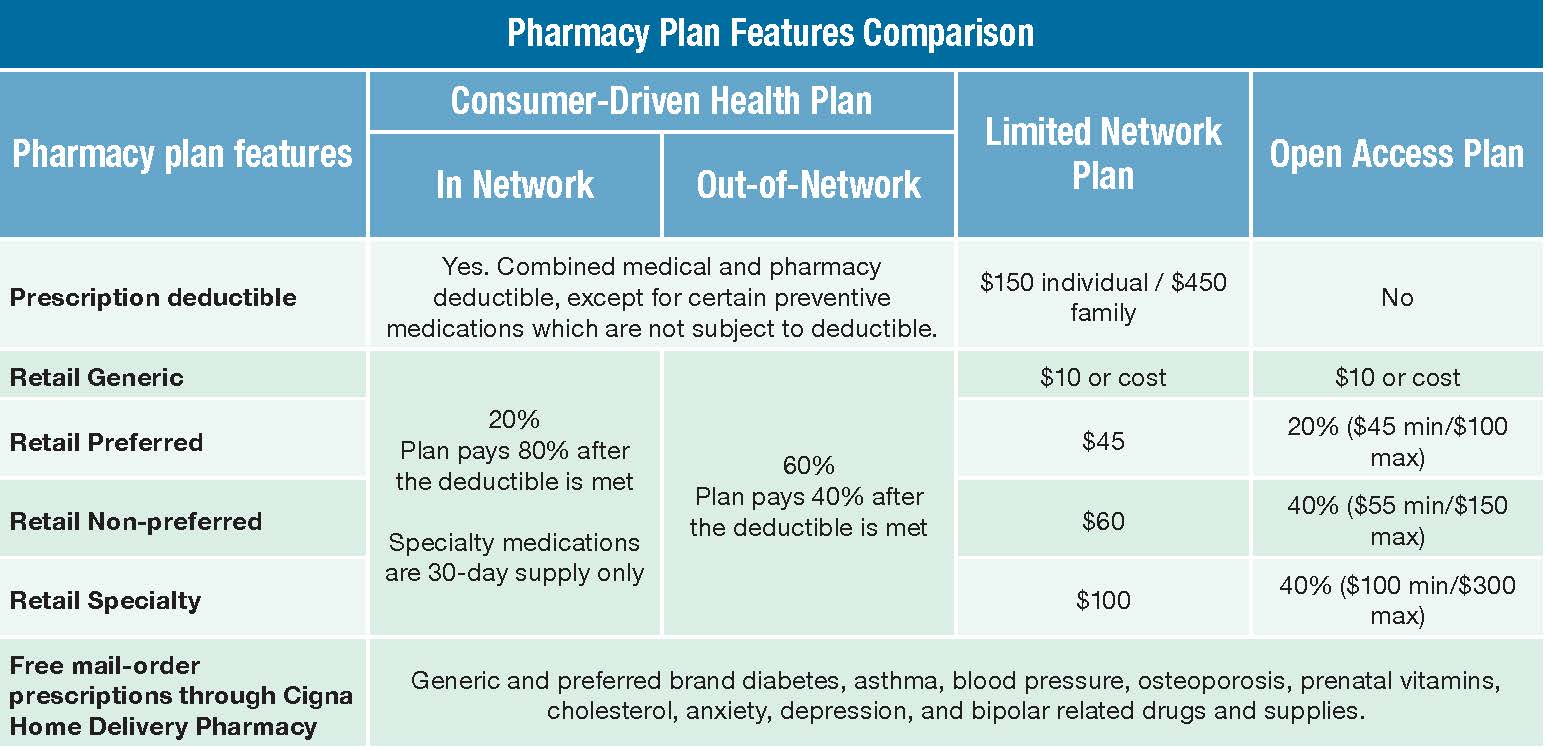
Participating Pharmacies: 30-day
- CVS/Target
- H-E-B Pharmacy
- Kelsey-Seybold
- Walgreens
- Walmart
Participating Pharmacies: 90-day
- CVS/Target
- Walmart
Visit Cigna.com/Rx90network to see a complete list of pharmacies in your network.
Need more information?
Current Plan Document for Limited Pharmacy
Cigna Value Four Tier Prescription Drug List
Cigna 90 Now Program
Cigna Preventative Medication Program
Express Scripts Pharmacy – Home Delivery
Express Scripts Pharmacy – Home Delivery FAQs
Cigna Patient Assurance (Insulin) Program
Cigna Home Delivery Pharmacy LifeScan Blood Glucose Meter Customer Voucher
PPACA No Cost Share Preventive Medications List Jan 2023
Free Medications
If you use Cigna Home Delivery, you can now fill the following prescriptions at no cost to you:
- Generic, and some brand name, asthma medications;
- Generic diabetic supplies;
- Brand name insulin;
- Generic cardiovascular and high blood pressure medications;
- Generic cholesterol medications.
*Not all prescriptions are available with Express scripts (formerly Cigna Home Delivery) services.
